
The alleged second wave of the pandemic started in February-March 2021 as COVID cases started climbing even when the vaccination drive is in full force. Many States have seen a considerable hike in COVID positive cases which has prompted them to take serious actions to stop the spread of the infection. Even health insurance companies are reeling under the heavy claim burden brought on by increased COVID related claims.
Insurance companies reported receiving increasing COVID-related claims from July 2020. Have a look at the claim trajectory –
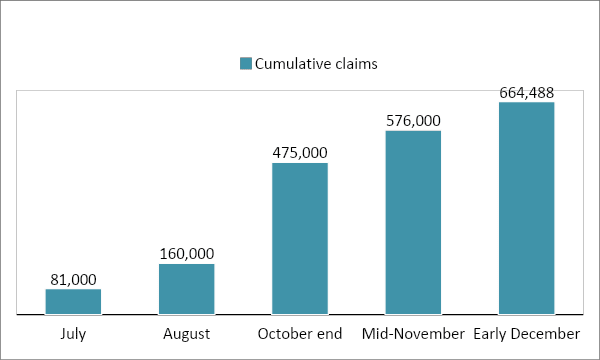
Source: Business Standard
As you can see, the number of claims started with 81,000 in July 2020 and climbed beyond 6.5 lakhs by December 2020. The total claim amount the companies settled during this period amounted to INR 9989.89 crores.
Talking about the current year, there has been a fresh surge in COVID cases and claims have started rising. As of 25th February 2021, companies have received more than 9 lakh claims related to COVID which amount to INR 13, 752.41 crores, as per GIC’s compiled data. Out of the claims that insurance companies have received, more than 7.6 lakh claims have been settled amounting to INR 7141.33 crores. This figure is close to 15% of the total health insurance premiums that the companies had collected till January 2021. The average claim settlement amounts to INR 93, 758.17 per claim.
Source: Business Standard
What so the insurance companies say?
Many insurance companies are stating that the number of claim settlements did not reduce despite the reduction in COVID cases towards the end of 2020. This is because many claims were reported on a reimbursement basis wherein the insurance companies need time to assess, analyse and settle the claims. So, even as COVID cases were declining in the last months of 2020, the claim settlements were not because of the payment of reimbursement claims. This is also the cause for the gap in the number of claims reported vis-à-vis the number of claims settled.
Impact on insurance companies
The high claim volume is distressing for companies as it impacts their profitability. With COVID specific health insurance plans becoming popular, insurance companies might face more claims if the COVID cases continue to rise despite the vaccination.
The true picture would become clear only after the pandemic subsides but for now, the high claim volumes are becoming a cause of concern for insurance companies. This might also convert to an increased premium in the coming years if the claim burden does not reduce.
Impact on policyholders
The claim experience of insurance companies does not affect you, the policyholder. In the case of genuine claims, insurance companies are bound to settle the claims within the prescribed time limits to avoid penal interests. So, if you suffer a COVID related claim, you would get a settlement for the claim if it is covered under your health insurance plan, whatever is the claim experience of the insurer.
However, if the premiums are revised, then you might feel a higher pocket pinch when you renew or buy a new health insurance plan.
The pandemic has been a rocky road for individuals and companies alike. Though it has resulted in higher claims, health insurance companies are also banking on the popularity and demand of health insurance plans, especially COVID insurance plans. A high claim volume is a short term phenomenon specific to the pandemic and as the pandemic subsides, things would settle down. Till then, insurance companies need to battle out the claims that they get.
































